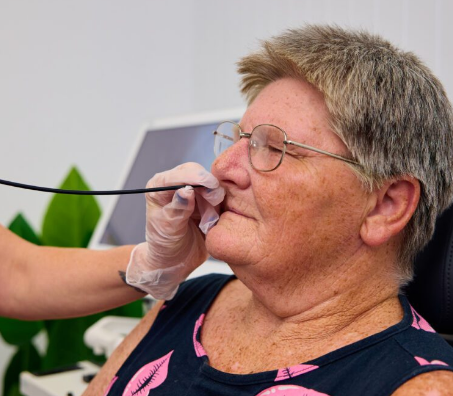
Swallowing
Hastings Macleay Speech Pathology has expertise in the assessment and management of swallowing disorders. Swallowing difficulty is termed 'dysphagia' and we can help by assessing someone's mealtimes, swallow function and provide recommendations for ongoing management. We have specialised objective assessments called Flexible Endoscopic Evaluation of Swallow (FEES) and Videofluoroscopic Swallow Studies (VFSS) that we perform with people to give us more detailed and specific information about someone's swallowing.
HM Speech can look at swallowing in adults and aged care clients, or perform feeding assessments on babies and children.
Swallowing is a complex process. Some 50 pairs of muscles and many nerves work to receive food into the mouth, prepare it, and move it from the mouth to the stomach. This happens in three stages. Speech Pathologists work with the first two phases, and sometimes assist Gastroenterologists with diagnosis in the third phase, the oesophageal phase.
During the first stage, called the oral phase, the tongue collects the food or liquid, making it ready for swallowing. The tongue and jaw move solid food around in the mouth so it can be chewed. Chewing makes solid food the right size and texture to swallow by mixing the food with saliva.

About Swallowing
Saliva softens and moistens the food to make swallowing easier. Normally, the only solid we swallow without chewing is in the form of a pill or capsule. Everything else that we swallow is in the form of a liquid, a puree, or a chewed solid.
The second stage begins when the tongue pushes the food or liquid to the back of the mouth. This triggers a swallowing response that passes the food through the pharynx, or throat (see figure). During this phase, called the pharyngeal phase, the larynx (voice box) closes tightly and breathing stops to prevent food or liquid from entering the airway and lungs.
Humans swallow roughly 900 times per day. People who have trouble swallowing are at risk of poor nutrition and hydration. Swallowing difficulties (dysphagia) are common in the following populations:
-
Cancer of the head and neck
-
Stroke (over half of people who have a stroke will develop swallowing difficulties)
-
The ageing process including loss of dentition, frailty, deconditioning or ill-fitting dentures
-
Dementia and other cognitive disorders
-
Degenerative diseases including Parkinson’s Disease or Motor Neuron Disease
-
Some autoimmune disorders including Scleroderma
-
Respiratory diseases including COPD
If someone you know presents with any of the following signs, it might mean they have dysphagia and early intervention is important:
-
Difficulty chewing certain foods
-
Holding food/drink or saliva in the mouth
-
Taking a really long time to get through a meal
-
Coughing when eating or drinking, or complaining of a “tickle” in the throat (aspiration)
-
Choking when eating or drinking
-
Complaining of food or drink sticking in the throat
The impact of dysphagia can be very detrimental to someone’s health. Some of the complications can include:
-
Aspiration pneumonia (chest infection caused by food/drink or saliva entering the lungs) recurrence can eventually lead to death
-
Aspiration pneumonia with recurrence can lead to significant morbidity and mortality
-
Dehydration and malnutrition
It is really important for early identification of dysphagia to avoid any adverse outcomes. At Hastings Macleay Speech Pathology we will provide a thorough assessment of swallowing and make it a priority to ensure eating and drinking is an enjoyable experience. Your safety is our priority and we will aim to eliminate risks of choking or developing a pneumonia and subsequently a visit to hospital.
Videofluoroscopy Swallow Studies
Videofluoroscopy Swallow Studies (VFSS) also known as Modified Barium Swallow (MBS) is an examination of swallowing done under x-ray.
A patient will be asked to eat and/or drink something while the speech pathologist views the oral and pharyngeal phase of swallowing. It is one of our gold standard assessment tools as it gives us a dynamic direct view of the structures used in swallowing. It helps to identify whether food or drink is going into the airway instead of the oesophagus, to recommend the appropriate food and drink to consume, and to develop rehabilitation strategies to improve swallowing function.
A VFSS is indicated when:
-
There is a need to observe oral preparatory, oral transit, pharyngeal, and/or oesophageal phases of swallowing;
-
a diagnosed or suspected presence of abnormalities in the anatomy of nasal, oral, pharyngeal, or upper oesophageal structures that would preclude endoscopic evaluations;
-
an aversion to having an endoscope inserted;
-
the presence of a respiratory disorder;
-
the presence of a persistent feeding refusal problem for which a swallowing disorder might be a contributing cause; or
-
the need to determine treatment or management strategies to minimise the risk of aspiration and increase swallow efficiency (Arvedson & Lefton-Greif, 1998).
About the Test:
A VFSS is done with your speech pathologist directing the assessment and a Radiographer taking the images. Most of the time, a Radiologist will also be present to assist with determining any abnormal anatomical structures and to make comment on physiology.
If you think you require one of these tests, call and speak with us today.


Flexible Endiscopic Evaluation of Swallow (FEES)
Hastings Macleay Speech Pathology Performs swallowing examinations using FEES which are a valuable tool for us to evaluate swallowing and guide the treatment of swallowing disorders (dysphagia). A FEES is a portable procedure that can be done in outpatient settings by passing an endoscope transnasally, allowing us to view the oropharynx, larynx & pharynx during swallowing.
A FEES differs from our alternative instrumental examination, a Videofluoroscopy Swallow Study, so if you are unsure of which one you or your patient requires, call us to find out more.